

Before setting off on a long trip, you need to get your vaccinations done. In this article, we’ll explain which diseases you need to protect yourself from, which vaccines to get, when and where to get them, and how much it costs…
This detailed article has been carefully and meticulously put together. It’s been proofread and corrected by a tropical diseases expert. However, you still need to go to an in-person appointment with a doctor, travel nurse or pharmacist specialising in travel medicine.
We carried out a large survey between 22nd and 24th November 2020 amongst 389 travellers. We asked them specific questions about their travels and vaccinations. The figures published in this article come from this survey. Learn more about our methodology
We don’t advise you to take the survey results as vaccination recommendations. When it comes to vaccinations, don’t just follow the crowd. Each traveller will have different needs, depending on their previous medical and vaccine history, their current general health, where they’re travelling to, how long for, and so on.
When planning a big multi-country trip beyond western countries, before anything else, you need to know your own vaccine record. You also need to make sure you’re up-to-date with any routine vaccinations in your day-to-day life in your home country.
To find out what vaccines you’ve already had, you should contact your GP practice (doctor’s office for Americans). They should have your entire medical history on file. If you’ve moved cities and changed GP practice, don’t worry – your health records should’ve been transferred when you signed up to your new practice.
If you’re travelling abroad, it’s strongly advised to be up-to-date with the recommended and routine vaccines in your home country, as they can be even more vital in other countries.
At this moment in time, there’s no mandatory vaccination scheme for people in the UK, it’s purely voluntary. Ultimately, it’s the parents or guardians who choose whether to get their child vaccinated or not, and adults for themselves.
However, the NHS strongly recommends getting vaccinations and routinely offers them to everyone free of charge.
Here’s the list of national routine vaccines in the UK. Given that they’re recommended and offered to babies, children, teenagers and adults free of charge, it’s highly likely you’ve already been vaccinated against these diseases:
To find out more about routine vaccinations, go to the NHS vaccinations and when to have them page. You’ll find the NHS vaccination schedule, which is broken down by age and recommended vaccines. You can click on each vaccine to learn more about it.
In the US, vaccination laws vary from one state to another. Some states are increasingly imposing vaccination requirements, particularly for certain professions, such as healthcare jobs.
Some states also require children attending public and private schools to be vaccinated. However, there are exemptions to this on the grounds of medical, philosophical, and religious reasons. To find out more, see the 2019 assessment, “State School Immunization Requirements and Vaccine Exemption Laws”.
Nonetheless, similar to the UK, the Centers for Disease Control and Prevention (CDC) in the US also recommends routine vaccines for everyone, to help fight vaccine-preventable diseases. But, it’s ultimately the parents or guardians who choose whether to get their child vaccinated or not.
Most health insurance plans cover the recommended vaccines at little or no cost. You can also still get vaccinated if you don’t have health insurance. And private health insurance usually covers you for the recommended vaccines. But, again, this can vary from one state or one insurance plan to another. You can visit the US Department of Health and Human Services (HHS) page to find out more.
Here’s the list of national routine vaccines in the US. Again, given that they’re recommended and offered to babies, children, teenagers and adults free of charge or for a small price, it’s highly likely you’ve already been vaccinated against these diseases:
To find out more about recommended vaccinations in the US, see the following vaccination schedules that are categorised by age: 0 to 6 years, 7 to 18 years old, and 19 years or older.
Some vaccines given in childhood, or later, require “booster” vaccinations throughout the course of your life. This helps to protect you against the virus for better and longer, as well as preventing the further spread of the virus.
The February 2022 UK routine immunisation schedule specifically shows at what ages to get each vaccine, from birth to 65 years old and older, as well as the ages at which to get your booster vaccinations.
It’s recommended to follow this vaccine schedule so that you’re best protected from potentially serious diseases, both in your home country and places abroad.
In the US, boosters are also part of the routine vaccines. They’re marked in the different vaccination schedules for infants and children, children and teenagers and adults.
Generally speaking, the average long-term traveller only needs some boosters, and they’re often the diphtheria, tetanus, polio and whooping cough vaccines.
NHS | NHS Digital | GOV.UK | UKHSA | Fit for Travel | CDC | HHS
In this section, we’ll go through all the diseases that travellers might face in high-risk areas, as well as the vaccinations recommended by the NHS and CDC to help protect you from them. It includes information on hepatitis A, hepatitis B, typhoid, yellow fever, Japanese encephalitis, rabies, tick-borne encephalitis, cholera and meningococcal meningitis (MenACWY). While hepatitis B and MenACWY are also part of the national routine vaccination schedules, they can also be considered as travel vaccines.
We compiled the following information using several official sources, including the NHS, Fit for Travel, Travel Health Pro, the World Health Organisation (WHO), the CDC and the United States Department of Health and Human Services (HHS).
When you travel for an extended period of time, the recommended vaccines vary from one person to another, and usually depend on the following criteria:
This disease is found everywhere in the world, but it’s much more common in countries with poor levels of sanitation. The WHO estimates that 90% of children who live in these areas are infected with the virus before the age of 10.
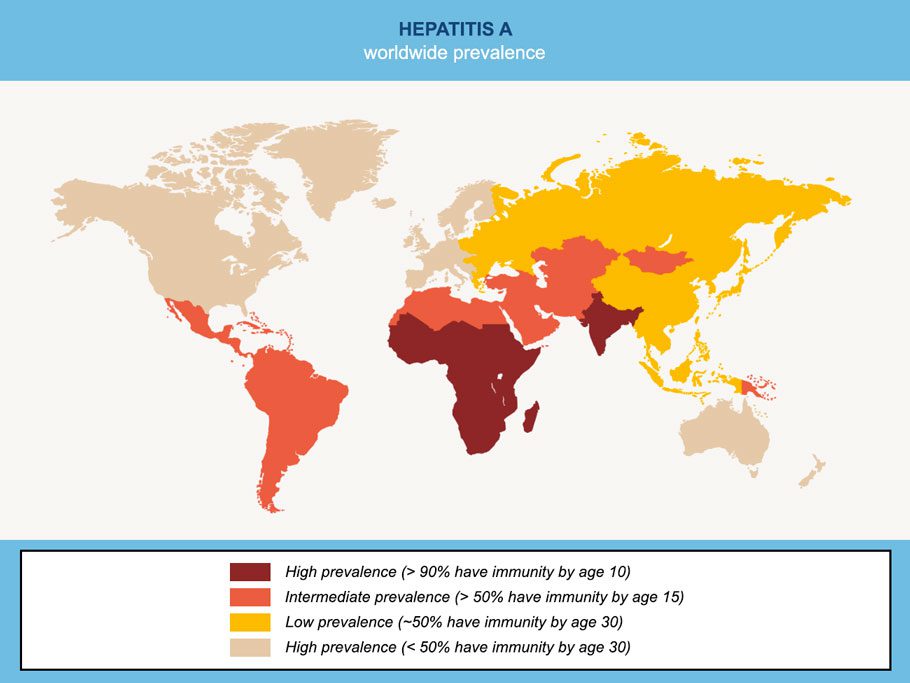

It’s a liver disease that can range from mild to severe. Its mortality rate is extremely low: 0.5%. Most infected people make a full recovery. In 60% of cases in children under the age of five and in 20% to 30% of adults, the infected person doesn’t have symptoms. Depending on the case, symptoms of hepatitis A can include a mild temperature, diarrhoea, feeling sick, sore tummy, dark wee and jaundice (yellowing of the skin and eyes). Recovery can last several weeks or even months. Once you’re better, you usually develop life-long immunity against it.
It’s spread in the poo of an infected person. You mainly catch it by swallowing food or drink that’s contaminated with the virus.
The vaccination is highly recommended for travellers from the age of 1 (from 6 months of age in the US) who intend on visiting remote areas with poor levels of satiation and hygiene, and where hepatitis A infection is common.
A single-dose vaccine is administered in the UK and US (Havrix and VAQTA, and Avaxim in the UK only). The first dose must be given at least two or three weeks before you leave, but it can be given on your departure day. The first dose provides adequate protection for the length of your trip.
The booster is recommended if you want life-long protection (20 years). You must get it six to 36 months later, depending on your age and the “type” of vaccine that’s been administered. For example, the Avaxim vaccine may be administered up to 36 months after the first dose. Vaccination is possible from the age of one.
In the UK and US, there’s also a combined vaccine for hepatitis A and hepatitis B (Twinrix), as well as a combined vaccine for hepatitis A and typhoid in the UK (ViATIM – not licensed in the US).
318 respondents said they’d travelled in a hepatitis A risk area: 31 were already vaccinated (unrelated to their trip), 69% were specifically vaccinated for their trip, 14% weren’t vaccinated, 4% couldn’t remember.
In 2019, according to the WHO, 296 million people were living with chronic hepatitis B worldwide, and this resulted in 820,000 deaths. There were also an estimated 1.5 million new infections annually.
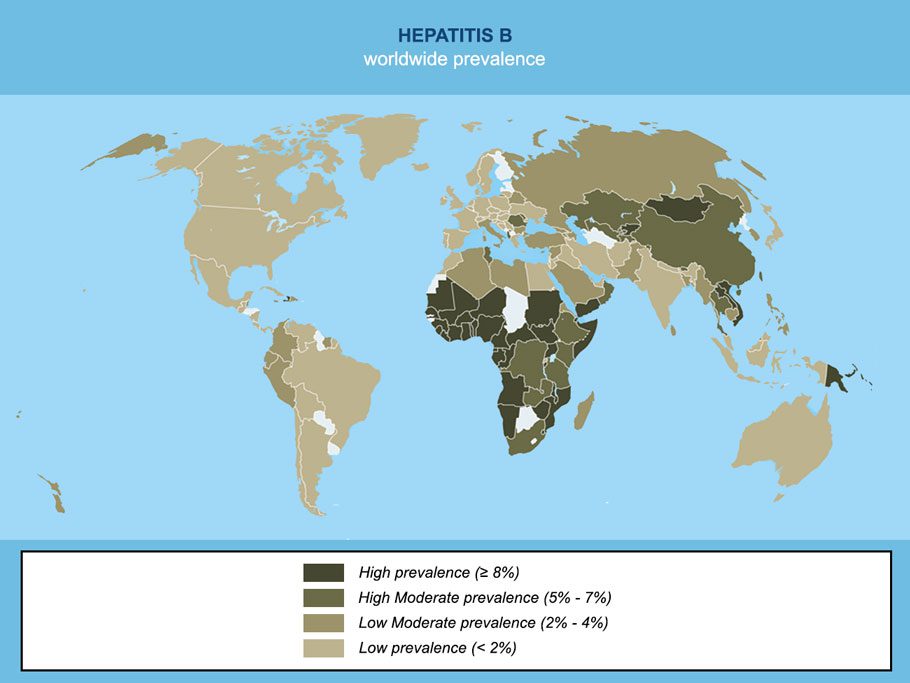

It’s an infection of the liver caused by a virus that potentially requires lifelong treatment if you develop a chronic infection. Among those infected, 90% are babies under one year old, 30% to 50% are children under six years old, and 5% of infected adults (who are fit and healthy) later develop a chronic infection. For 20% to 30% of adults with a chronic infection, it could eventually lead to scarring of the liver (cirrhosis) or liver cancer.
From mother to child. Used needles (medical equipment, syringes, tattooing, body piercings, and so on). Blood, saliva, vaginal and seminal secretions, unprotected sexual intercourse.
Recommended for all travellers going to infected areas for an extended period of time.
The vaccines used in the UK and US consist of three doses. The second dose one month after the first, then a third dose six months after the first. On an accelerated schedule, the course can be done one month before departure. On this accelerated schedule, a fourth dose is recommended 12 months later, if you’re still at risk of exposure.
In the US, they also administer a two dose vaccine (Heplisav-B), the second dose given one month after the first.
In the UK and US, there’s also a combined hepatitis A and hepatitis B vaccine (Twinrix).
292 respondents stated they’d travelled in an area at-risk of hepatitis B. 40% were already vaccinated (unrelated to their trip) and 42% were specifically vaccinated for their trip. 18% didn’t get vaccinated.
This disease has almost entirely disappeared in industrialised countries. However, it’s still pretty common in countries that have poor sanitation and limited access to clean water. In 2018, the WHO estimated that typhoid infected between 11 and 20 million people and caused up to 160,000 deaths worldwide each year. The UK Health Security Agency (UKHSA) states that typhoid is uncommon in the UK. There are an estimated 500 cases diagnosed each year, but most of these people became infected whilst travelling abroad.
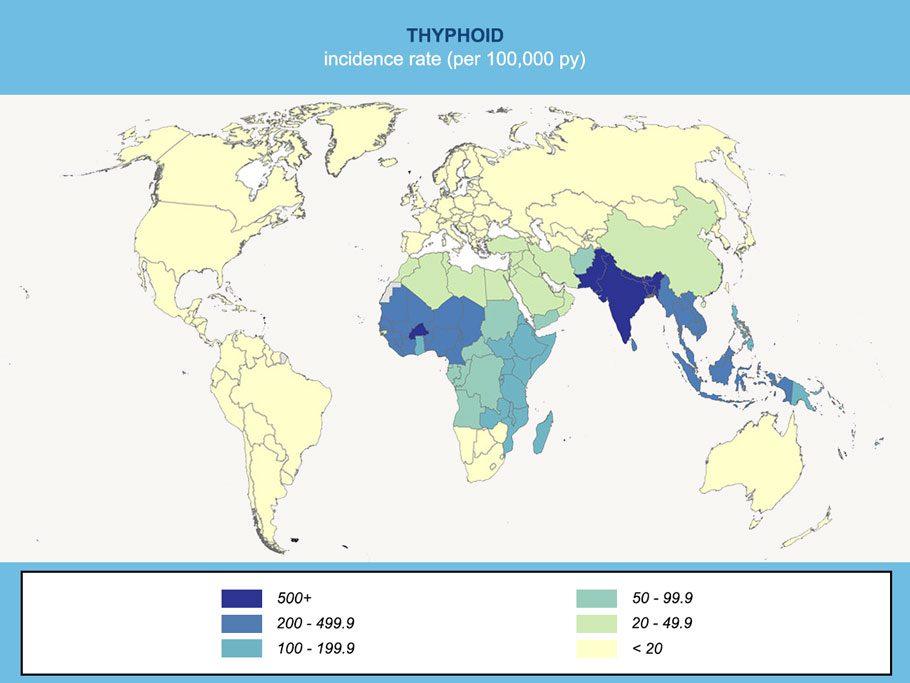

It’s a bacterial infection that can range from mild to severe. The symptoms of this infection can last for several weeks and include a persistent high temperature, general aches and pains, sore tummy with diarrhoea or constipation and, in the most severe cases, problems linked to the heart, intestine and nervous system. In the most severe cases, and if it’s not treated, or if the strain of the virus is resistant to the antibiotics, it has a 10% death rate. If the disease is well treated, the death rate lowers to 1%.
Mostly by drinking water or food that’s been contaminated with infected poo or wee, or directly from person to person. A small percentage of individuals who recover from typhoid fever may continue to host the virus and subsequently spread it.
Vaccinations are recommended for anyone travelling to parts of the world with poor sanitation levels or where typhoid fever is common, such as the Indian subcontinent and Africa, as well as areas in South and Southeast Asia, South America and the Middle East.
In the UK and US, the licensed vaccine is a single jab (Typhim Vi). Ideally, you should get it at least one month before you travel, but this can be shortened to 15 days. Protection lasts for two to three years. So, you’ll need a booster if you go on another trip in a high-risk area. There’s a 60% protection rate in endemic areas. You must be two years and older to get this vaccine.
Another licensed vaccine comes in the form of oral capsules (Vivotif). In the UK, you must take three capsules every two days in a five-day period. Protection starts around seven to 10 days after taking all three capsules. You must be five years and older to take them.
In the US, they administer the same oral vaccine. But, you must take four pills every other day and aim to finish them at least one week before travel. You must be six years and older to take them. It requires a booster every five years.
In the UK, there’s also a licensed single dose of a combined hepatitis A and typhoid vaccine (ViATIM). Protection starts around 14 days after the injection. Protection against hepatitis A lasts for one year and protection against typhoid lasts for three years. So, if you later plan on travelling in hepatitis A / typhoid-risk areas, remember to get your boosters. You must be 15 years and older to get this vaccine.
306 respondents said they’d travelled in an at-risk of typhoid. Amongst them, 65% were vaccinated, 27% weren’t vaccinated and 8% couldn’t remember.
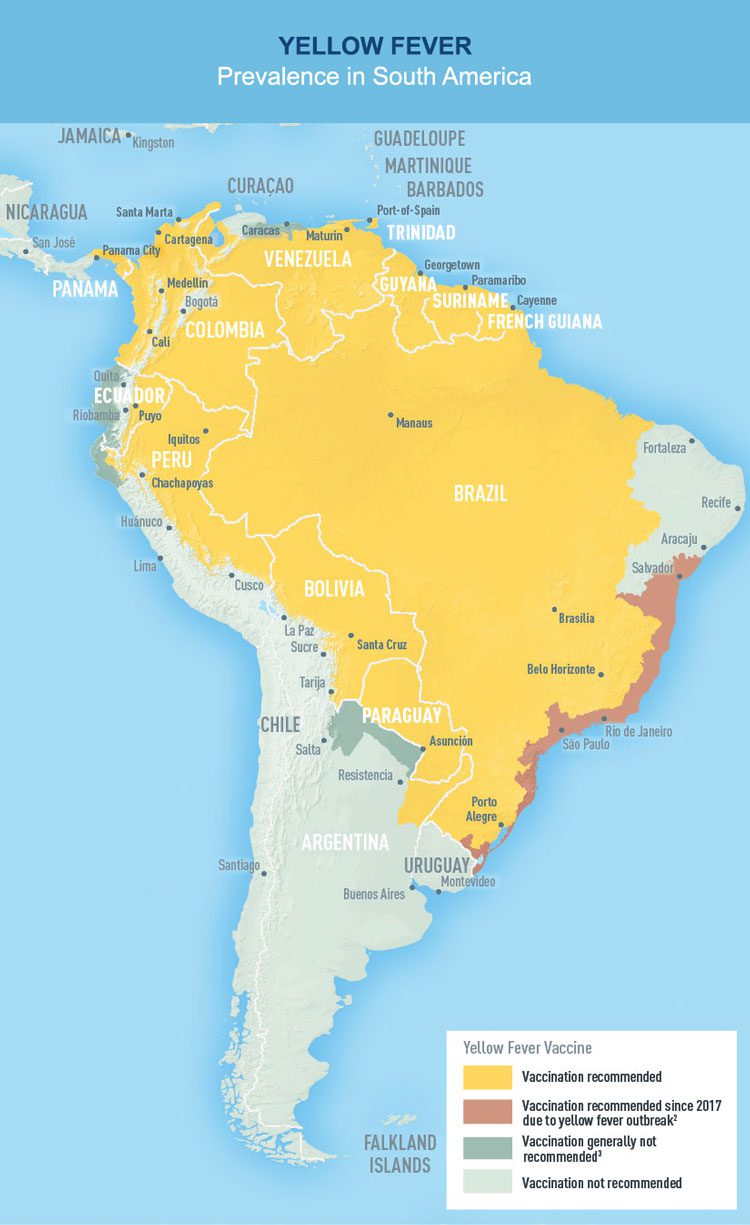
Yellow fever is found in most African and Latin American countries, as well as Trinidad in the Caribbean. But, 90% of cases are reported in Sub-Saharan Africa. 200,000 people are affected globally every year and around 30,000 die from it.
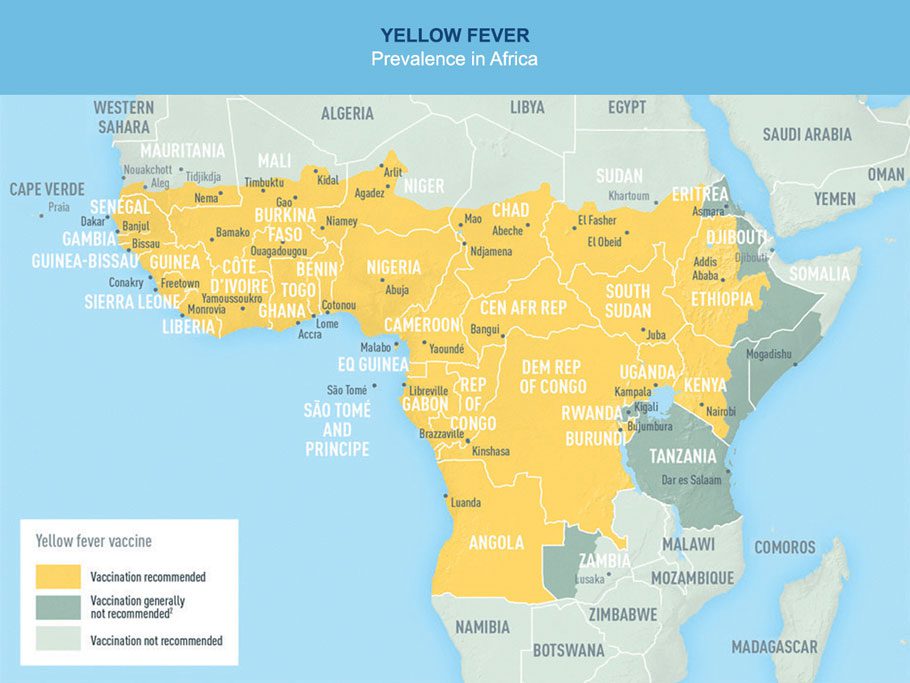


Yellow fever is a disease caused by a virus. In 85% of cases, it doesn’t cause any symptoms and you recover from it without even realising. When symptoms appear (fever, nausea, vomiting, headache, etc.), they usually disappear after three to four days.
However, for a small proportion of those infected, the disease becomes more severe, attacking the liver and kidneys. Symptoms include yellowing of the skin and eyes, also known as jaundice. Half of those that develop severe disease die from it within seven to 10 days. While the disease can’t be directly treated itself, the symptoms can, and this is what reduces the risk of death.
The virus is transmitted when a mosquito, most often the Aedes species, bites an infected human or monkey, and then bites another human. Mosquitoes can pass the virus onto their offspring.
It’s recommended for travellers going to areas where the virus is present. It’s not recommended for pregnant or breastfeeding women and babies under nine months of age.
Many countries require you to provide proof of a yellow fever vaccination to enter their country. Sometimes, the requirement only concerns travellers coming from a country where yellow fever is endemic. So, you need to have your yellow fever vaccination certificate, also known as an International Certificate of Vaccination of Prophylaxis (ICVP).
The WHO has drawn up a list of countries with risk of yellow fever transmission and those requiring proof of vaccination.
You need one dose at least 10 days before travelling. It usually provides lifelong protection in most people. However, in some particular cases, you’ll need a booster dose. For example, if you were previously vaccinated when you were pregnant or were under two years old. Vaccination is possible from nine months old.
This vaccine is a live, weakened form of the virus itself, so the vaccination is only available from registered yellow fever vaccination centres. See list of registered yellow fever vaccination centres in England, Wales and Northern Ireland here, the list for Scotland here, and finally the list for the US here.
199 respondents said they’d travelled in an area where there’s yellow fever. Amongst them: 89% were vaccinated, 9% weren’t vaccinated, 2% couldn’t remember.
There’s an estimated 68,000 serious cases of Japanese encephalitis globally each year, with around 13,600 to 20,400 deaths.

Japanese encephalitis is a viral infection related to dengue and yellow fever viruses. Most cases are mild. Infected people display symptoms of fever, headache, or don’t have any symptoms at all. Around 1 in 250 of infected people develop severe symptoms, resulting in infection and inflammation of the brain (encephalitis). About 30% of those with severe symptoms die, and amongst the 70% of survivors, around 15% to 20% of them will be left with permanent brain damage. There’s no cure for the infection. Treatment only relieves the symptoms.
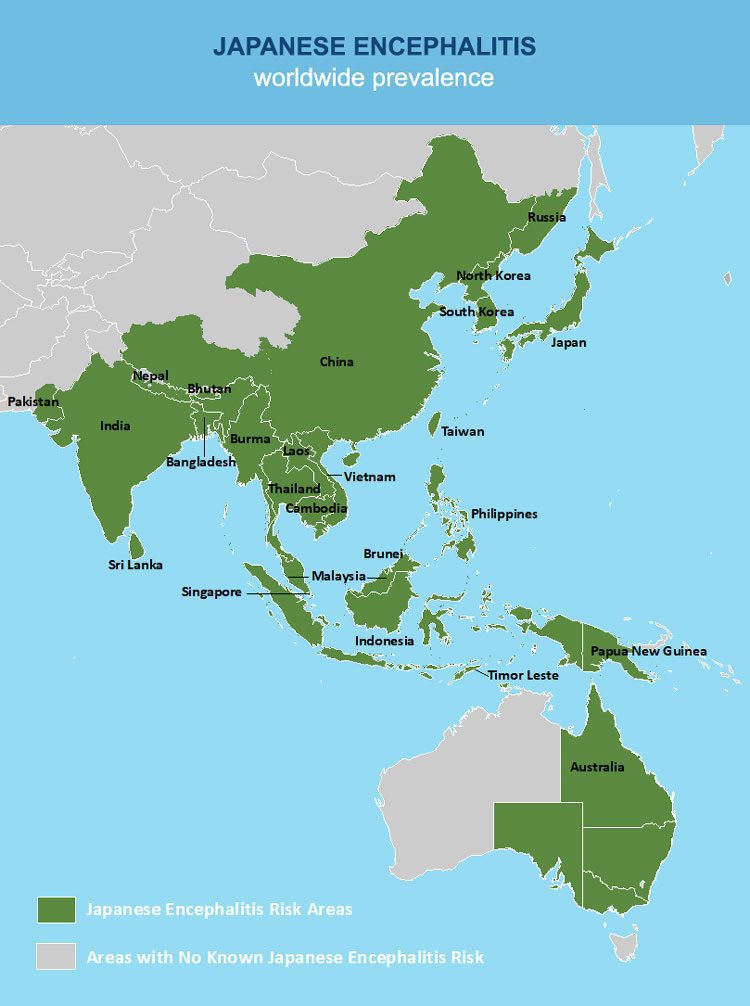
The virus is spread through mosquito bites in some countries in Southeast Asia and the Pacific Islands. It’s most common in rural areas, farming areas, particularly around rice fields and where there are pigs. Mosquitoes are actually infected first, when they bite an infected mammal. There’s a risk all year round in tropical climates, but the risk increases during the rainy season and summertime in mild regions.
Travellers are rarely affected by this disease. The vaccine is only recommended to those who’re planning a long stay in countries where there’s a risk of getting the virus and are going there during the most risky periods, like the rainy season. It’s also recommended to those who’re doing lots of outdoor activities in high-risk areas (camping, hiking, etc.)..
It includes two jabs spaced 28 days apart. With this vaccine (IXIARO), on a licensed accelerated schedule, adults aged 18 to 64 years can get the second dose seven days after the first. This accelerated schedule can also be considered for children aged two months to 17 years old and those over 65 years old, but it’ll be “off licence”.
In any case, the second dose should be completed at least seven days before you go to an area where there’s a risk of the virus. A booster dose is recommended 12 to 24 months after the first vaccination if there’s a continued risk for infection or reexposure.
276 respondents said they’d travelled in an area where there was a risk of the virus
Watch out - travelling to an area where there’s a risk of the virus doesn’t mean you have to get the vaccination (see “Recommended Vaccination” above)
. Amongst them: 43% were vaccinated against Japanese encephalitis, 55% weren’t vaccinated and 2% couldn’t remember.
Nearly 59,000 people die from rabies every year. 15 million people are treated after being bitten by an animal suspected of carrying rabies. 95% of fatal cases worldwide occur in Asia and Africa.

Rabies is a viral infection. It’s present in the saliva of infected animals. It causes a fever and affects the brain and nerves. Symptoms usually start three to 10 weeks after exposure, but can also sometimes start in less than a week. Once symptoms appear, it’s too late, rabies is almost always fatal. If an infected person is treated quickly and correctly, before having symptoms, 99.999% of the time they recover from the viral disease without experiencing any symptoms.
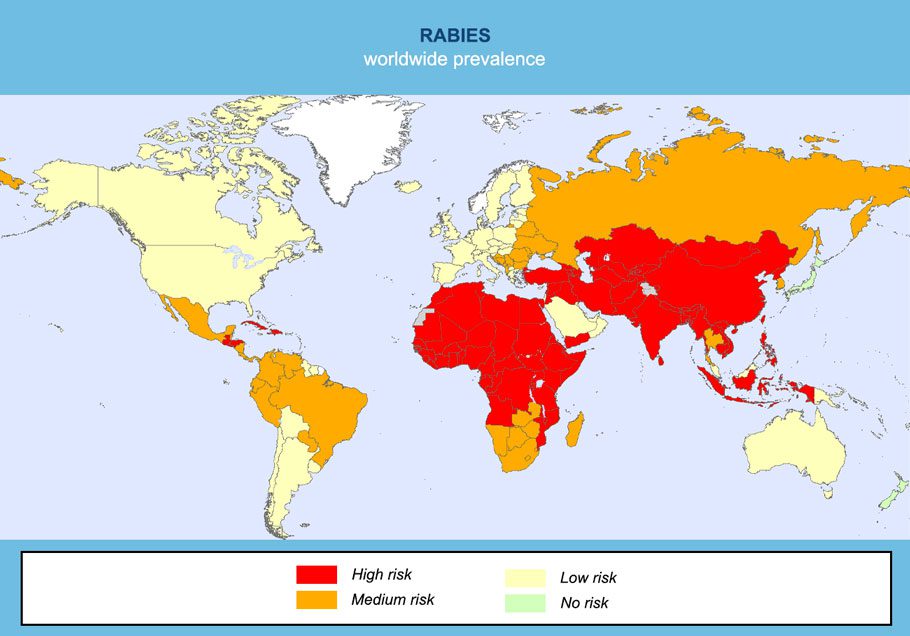
If an infected animal bites you, licks on a fresh wound or scratches you. All mammals can potentially carry rabies, but dogs, bats, skunks, cats and racoons are the main carriers. In America, bats are the main cause of infection. Elsewhere, in 95% of cases, it’s dogs.
You can never quite know if the animal in question is really infected with rabies or not. If you’re unsure, you should always seek post-exposure treatment as quickly as possible.
The rabies vaccine helps protect you against the rabies virus, but it’s not 100% effective. So, there’s still a risk of being infected if you’ve been bitten, scratched or licked by a rabid animal. If you’ve been (or think you might’ve been) exposed to rabies, even if you’re vaccinated, you need to undergo post-exposure treatment immediately.
If you’ve already been vaccinated against rabies, you’ll be given two extra doses of the rabies vaccine over three days.
If you haven’t already been vaccinated, you’ll usually be given four doses of the rabies vaccine over a period of three weeks. You’re also sometimes given a specialised medicine, “Human Rabies Immunoglobulin (HRIG),” which should be given as soon as possible after exposure. However, HRIG treatment often isn’t a viable option, especially in underdeveloped areas of the world, hence the importance of being vaccinated beforehand.
The vaccination is recommended for all those travelling to high-risk areas, but especially for young children who’re starting to walk, as they’re more likely to be bitten than adults.
In the UK, they administer a full pre-exposure course of rabies vaccines. It includes three doses given over a period of 21 to 28 days. An accelerated vaccination schedule is possible, where the three doses are given over seven days, but this option is only available for adults. The vaccine protects you for 10 years. It’s also available for pregnant women and babies who’re starting to walk.
In the US, as of May 2022, they now have a two-dose vaccination schedule that protects for up to three years. The second dose should be given seven days after the first. This is usually followed by a booster dose three weeks to three years after the first vaccine (depending on your situation). Or, a one-time titer check (a blood test to check for the presence of bacteria or a disease), one to three years after the first vaccine.
319 respondents travelled in a country with an orange or red risk of rabies exposure (see map above). Amongst them: 49% were vaccinated, 48% weren’t vaccinated and 3% couldn’t remember.
32 respondents only travelled to an area with a moderate-risk of rabies exposure (orange on the map). This is the case for most Latin American countries. Amongst them: 53% were vaccinated and 43% weren’t vaccinated.
17 people were bitten or scratched by an animal hard enough that they bled. 9 by a dog and 8 by a monkey. All were in a red zone, in Southeast Asia. 10 of them had post-exposure treatment. When their travel plans included many countries, sometimes they started the treatment in the country where the incident happened and continued it in another country.
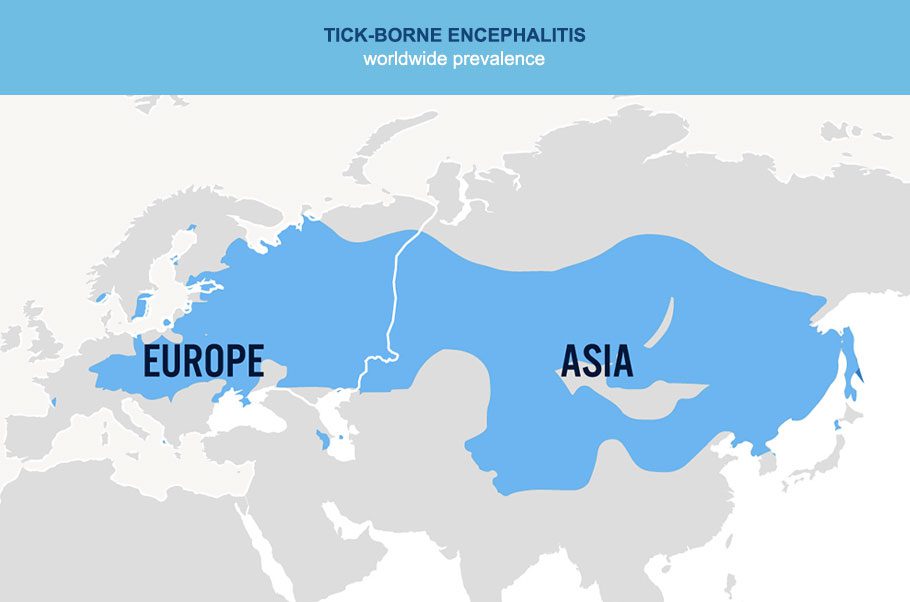
When you’re outdoors, in rural or woodland areas, from spring to autumn, at an altitude of at least 1,500 metres, in Eastern Europe, Russia, Northern China, Mongolia, South Korea, Japan and Kyrgyzstan. There are 5,000 to 13,000 reported cases each year worldwide.

This disease is caused by a virus. It starts with flu-like symptoms. Encephalitis breaks out in 20% to 30% of cases, meaning that the brain is affected. The infection of the central nervous system can cause mental and physical health conditions. 1% to 2% of people with encephalitis die from it and 10% to 20% have long-term neurological problems. There’s no treatment for it, you can only relieve the symptoms.
It’s spread by tick bites from infected ticks.
The vaccination is recommended for all travellers from the age of one who’re travelling to risk areas.
Ideally, you should start the vaccination course six months before departure. You need three injections to be protected for three years. You should have the second dose one to three months after the first, and the third dose five to twelve months after the second.
On an accelerated schedule, with the TicoVac vaccine, you can get the second dose two weeks after the first. Two doses provide sufficient protection for the ongoing tick season. But, you still need the third dose five to twelve months later to prolong the protection. So, you could do this when you return from your trip, as long as it’s 12 months later or less.
The WHO estimates that there are 1.3 to 4.0 million cases of cholera each year worldwide and 21,000 to 143,000 subsequent deaths. The disease is found worldwide, but it’s more common in countries with poor levels of sanitation and poor access to clean drinking water, such as Africa, India and Southeast Asia. However, as a traveller, the chances of getting it are extremely low.
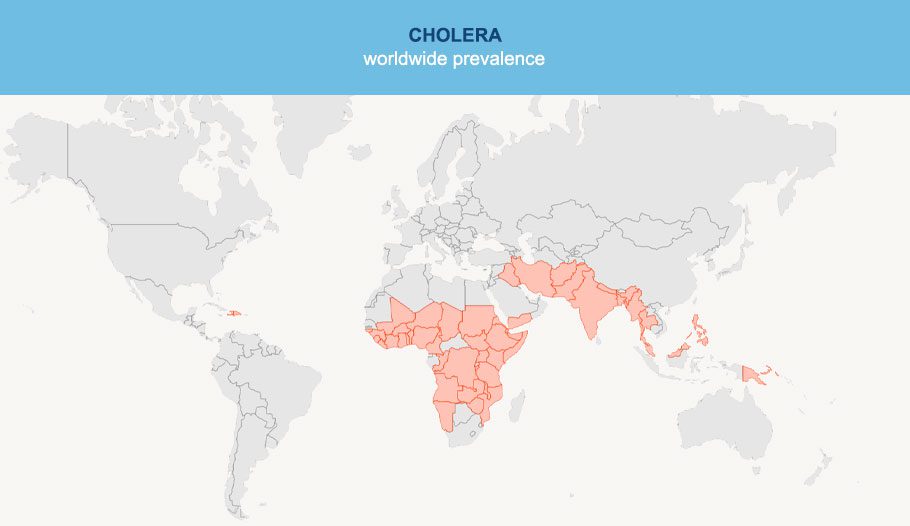

It’s an infection that can cause acute diarrhoea, leading to severe dehydration. In healthy individuals, 75% of those affected have mild or no symptoms at all. Symptoms can appear 12 hours to five days after exposure.
It’s transmitted by ingesting food or water that’s been contaminated.
An oral vaccine is available in the UK, and a different oral vaccine in the US. But, most travellers don’t need it as there’s only a small risk of catching it. However, the vaccine is sometimes recommended for travellers going to a high-risk and / or remote area with active cholera transmission. Or, for humanitarian aid workers going to an area where cholera outbreaks are likely.
In the UK, they administer an oral vaccine (Dukoral). Adults take two doses, one to six weeks apart. Children aged two to six years should take a third dose one to six weeks after the second. In both cases, the final dose should be taken at least one week before your departure. The adult vaccine provides protection for up to two years, and the child vaccine, six months.
In the US, they have a single-dose vaccine (Vaxchora) available for 18 to 64 year olds. It should be taken at least 10 days before potential exposure. The duration of protection is around three months.
The disease is found all around the world, but predominantly in the Sahel region, between Senegal and Ethiopia. There are nearly 30,000 cases each year.
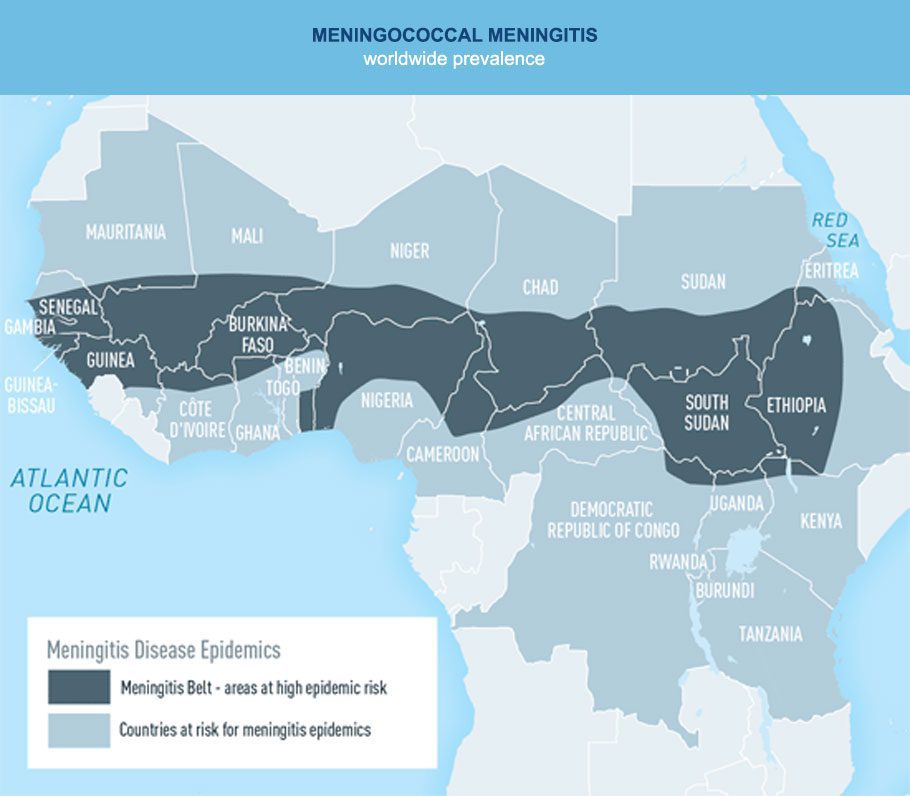

Meningitis is a disease that causes an infection of the membranes that surround the brain and / or septicaemia (blood poisoning). Symptoms can include intense headaches, fever, vomiting and various neurological problems. The disease is fatal in 50% of cases without treatment and in 5% to 10% of cases with treatment, even when the disease is treated quickly with quality care. Amongst those that survive, almost 20% have long-term neurological problems, such as hearing loss or seizures.
Meningitis can have several causes (viruses, bacteria, fungi, etc.). “Meningococcal” meningitis is caused by the bacteria of the same name.
The disease can be spread from person to person through saliva and respiratory secretions (kissing, spitting, sneezing, coughing, and so on).
There’s a low risk of infection for travellers. The vaccine is only recommended for long-stay travellers going to the Sahel belt region, who’ll be in close contact with the local population, like humanitarian aid workers.
Vaccination is mandatory for pilgrims travelling to Saudi Arabia and you must provide proof of this. This is because the disease could spread rapidly amongst the masses and cause a public health crisis.
There are several vaccines against meningococcal meningitis. In fact, we know 12 types of meningococci (that is to say, serogroups). Each of these types is classified by a different letter and requires a different vaccine. Not all types pose the same risk nor in the same places.
In the UK, most babies get the MenB and MenC vaccines as part of the NHS vaccination schedule. However, regardless of whether you’ve had the MenC vaccine when you were younger or not, you should still get the MenACWY vaccine if you plan on travelling to areas with a high risk of infection.
The MenACWY vaccine, also known as the quadrivalent meningococcal meningitis vaccine, offers protection against 4 types of bacteria that can cause meningitis: meningococcal groups A, C, W and Y. It consists of a single injection that should be given two to three weeks before your departure. Babies one year old and under need two doses. The second dose should be given one month after the first.
In the UK, the MenACWY vaccine has routinely been offered to teenagers in school Years 9 and 10 since 2015.
In the US, 11 to 12 year olds are advised to get the vaccine, with a booster dose at 16 years old.
44 respondents said they’d travelled in a country where there was a risk of meningococcal meningitis (A, C, Y, W). 14 of them were vaccinated. However, we don’t know how long they spent there, nor how close they were to the local population.
Adding a country by country summary table to this article wouldn’t have been that useful, as there are plenty of tools and resources out there that already summarise all the key travel and health information you need to know.
Fit for Travel is just one of those great resources. The Destinations page allows you to look up specific travel health information and requirements for each country. When you click on a country, you get all the health advice, from COVID-19 to recommended vaccinations. The information is presented clearly and is all up-to-date.
Travel Health Pro, which incorporates the travel health resources of the National Travel Health Network and Centre (NaTHNaC), works very similarly to Fit for Travel. The Country Information page displays countries from A to Z. When you click on a specific country, the travel health information is broken down into different sections: General information, Vaccine recommendations, Malaria, other risks, COVID-19, and Important News. Therefore, you can quickly and easily navigate your way around.
It also has a World Overview that allows you to see the latest news and disease outbreaks pinpointed on a world map. This information is sourced from credible agencies, such as the CDC and the WHO.
The Green Book, also known as Immunisation Against Infectious Diseases, provides up-to-date information on vaccines and vaccination procedures in the UK. It comes from the UK Health Security Agency (UKHSA) and is designed for public health professionals. Therefore, it’s detailed, pretty long and contains scientific jargon. What’s more, it doesn’t provide country-by-country information.
However, if you want to know the ins and outs of diseases, vaccinations and vaccines, this is the place to look. It’s available in PDF format on the GOV.UK website. The interactive contents page is particularly useful, as you can jump to the relevant chapter. For example, if you want to know all about Japanese encephalitis, you can click on Japanese encephalitis: the green book, chapter 20 and you’ll be directed to this specific chapter. Therefore, you don’t have to waste time scrolling through the entire PDF.
The Centers for Disease Control and Prevention (CDC) is the national public health agency of the United States and is another great source for country-specific information related to vaccines and immunisations.
If you head to the Destinations page, you’ll find a complete list of countries. When you click on a country you’ll be taken to a specific page. Similar to Fit for Travel and Travel Health Pro, you’ll find different sections, from Travel Health Notices to Vaccines and Medicines. There’s even an After Your Trip section.
What’s particularly handy about this website is the vaccines and medicines table. It clearly and simply details key information, such as routine vaccines you should be up-to-date with and the recommended vaccines for that specific country. If you want to find out more about each vaccine, you can click on the hyperlink. There’s also a table for non-vaccine-preventable diseases.
The International Society of Travel Medicine is committed to promoting healthy, safe and responsible travel worldwide. In their Global Travel Clinic Directory, you can find all the ISTM members who operate in travel clinics where they offer pre-travel immunizations, guidance and medicine to help protect you while travelling.
What’s great about the directory is that you can narrow your search by using the listed criteria. For example, you can search by country and see all the relevant travel clinics. Or, you can tick a particular service you’re looking for, such as “Pre Exposure Rabies Vaccinations”, and so on.
The Vaccine Hub is another great resource for information related to vaccine-preventable diseases, travel health and immunisation. Being an Australian website, some of the tools are more geared towards Australian citizens and their national immunisation program schedule.
Nonetheless, it comprises the key travel health information for each country via an Interactive Travel Map. It’s very user-friendly: you scroll around the globe, click on a specific country, and up pops vaccine advice for travellers. The information is clear, up-to-date and based on information from the CDC and Smartraveller.
Perhaps a minor drawback is that it only provides specific travel health information for the most popular destinations.
The CDC Yellow Book is a source for health professionals who provide healthcare to international travellers. It has all the latest information on pre-travel vaccines, vaccine recommendations and country-specific health advice. This information comes from hundreds of travel medicine specialists. The whole book can be accessed online. Its interactive contents page allows you to quickly find the topics that are relevant to you.
Finally, if you really want to be up-to-date with the latest vaccine news in the UK, you can look at the Vaccine update from the UKHSA. It’s updated any time there’s a change relating to vaccines, so you can expect monthly or even weekly issues. Like “The Green Book”, it’s designed for health professionals, so it’s pretty detailed. That said, there’s a contents page that helps you easily see whether there are subjects that concern you or not.
Below you’ll find a summary of the vaccination deadlines for “travel vaccines”. The vaccination days are shown as if you were to do the last vaccinations on the day of departure, which is obviously a really bad idea. Ideally, you should plan a few days or even a few weeks ahead to avoid stressing yourself out in the pre-departure phase.
What’s more, by taking care of it ahead of time, it’s easier to set up a time-saving, and even money-saving, vaccination schedule, as you can group as many jabs as possible on the same day.
If you go about it in a “rushed” way, you may still be able to do it “in time”. Indeed, some vaccines can be done on an “accelerated” schedule, but they often have additional constraints. We’ll explain this later on in the chapter.
*Yellow fever, hepatitis A, typhoid, Japanese encephalitis and the first rabies injection can be done on the same day, at D-28.
**The ViATIM vaccine is a combined hepatitis A and typhoid vaccine administered in a single jab.
As with “standard” vaccines, “travel vaccines” also sometimes require boosters after the first jab for the protection to be effective for life, or at least to prolong its duration of protection. When there’s no booster, it means it provides lifelong protection.
*Hepatitis B: 4th dose required at 12 months
**Tick-borne encephalitis: with this accelerated schedule, you’re only protected for the ongoing tick season. To get fully vaccinated and be protected for 3 years, you’ll need a 3rd jab 5 to 12 months after the 2nd.
***Rabies: the US uses the same vaccines as the UK, but instead of 3 doses, they now only administer 2 doses (as of May 2022). If you follow the accelerated schedule, you’ll need a booster dose at 1 year in the UK, and within 3 years in the US
****Japanese encephalitis: booster dose required 12 to 24 months following the primary course; accelerated schedule only suitable for 18 to 65 year olds
Jane Chiodini is an experienced Travel Health Specialist Nurse in the UK. She told us everything about where to get vaccinated in UK for a long travel around the world:
If you plan on going on a long trip abroad, here are the reasons why it’s often easier to get all your vaccines done in a registered yellow fever travel vaccination clinic:
Every time a health-care provider vaccinates you, in your vaccines record card, they note down the date of the jab, the name of the vaccine and / or the batch number (on a small sticker), the next booster / revaccination date, and they stamp or sign it.
It’s a good way to remember the vaccinations you’ve already had done and the boosters you’ll need, so you can be up-to-date. Some people also use the International Certification of Vaccination or Prophylaxis (ICVP) booklet. While it’s specifically used for the yellow fever vaccine, it also has pages that can be used for other vaccinations.
You can ask for one from your GP, pharmacy or vaccination centre and it’s free.
When you get vaccinated against yellow fever (only in a registered vaccination centre), you’re given a yellow fever vaccination record, also known as an International Certificate of Vaccination or Prophylaxis (ICVP) or a Yellow Card. This is different to the standard vaccine record card. The health-care provider writes in the booklet, certifying that you’ve been vaccinated against yellow fever.
As mentioned above, on the following pages, you can also write all the other vaccinations you’ve had inside it.
If countries require you to be vaccinated against yellow fever before entering (see list of countries), you must show your Yellow Card as proof.
If you lose it, you run the risk of not knowing what vaccines and boosters you need to get done. What’s more, if you lose the ICVP, you won’t be able to prove that you’ve been vaccinated against yellow fever. This could be problematic when crossing borders into countries that require it.
If you got your vaccinations done at your GP, they should have kept a record of all the vaccines you’ve received. So, they can give you a new vaccine record card and rewrite the vaccinations in it.
If you lose your yellow fever certificate, you might be able to get another one reissued from the registered vaccination centre you went to. Ideally, you should be able to provide them with key details, such as the vaccination batch number and the date you had the vaccination. Therefore, it’s a good idea to note this information down in a safe place (just like you would, for example, your passport number) when you get the vaccinations done.
If you’ve completely lost track of your vaccines and can’t remember what you’ve had done at all, don’t worry! Repeating a vaccine that’s already been given is no more “dangerous” than getting vaccinated for the first time. You can also get a blood test at your GP practice or local hospital. The lab results will determine which diseases you have the antibodies for, and therefore which diseases you’re already been vaccinated against.
Getting vaccinated before a long, multi-country trip can be pretty costly and you’ll probably need to factor it into your budget.
An adult wanting to get most of the main vaccines that are recommended for travellers (hepatitis A, hepatitis B, Japanese encephalitis, meningococcal meningitis, rabies, tick-borne encephalitis, typhoid and yellow fever) will have to spend around £850 (and $3000 in the US).
Fortunately, it’s unlikely that you’ll need to be vaccinated against all of these diseases. And what’s more, the most expensive vaccines (like rabies, tick-borne encephalitis and Japanese encephalitis) are also those which are often the least recommended.
All vaccines that are part of the NHS routine immunisation schedule (diphtheria, tetanus, whooping cough, polio, HiB, hepatitis B, MenB, rotavirus, MenC, PCV, MMR, flu, HPV, MenACWY) are available free on the NHS.
Some travel vaccines are also free on the NHS if your GP surgery is signed up to provide travel vaccination services. If this is the case, you can get typhoid, hepatitis A and cholera vaccines for free.
Other travel vaccines may be available in your GP surgery, but as they’re for travel purposes, you’ll have to pay for them.
You’ll have to use a private service and pay for other travel vaccines: hepatitis B (depending on your GP practice and hepatitis B vaccination history), Japanese encephalitis, meningitis vaccines, rabies, tick-borne encephalitis, and yellow fever.
These can be done at your GP practice for a fee, or at private travel vaccination clinics or large pharmacy chain outlets, like Boots and Superdrug. Prices will vary depending on where you get them done. Sometimes you’re charged for the consultation and advice, the vaccine itself, the administration of the vaccine, or even all three.
For instance, if you just go for a medical consultation at a Superdrug Health Clinic or MASTA Travel Health Clinic, and don’t purchase a vaccine, you’ll be charged a fee of £20. Whereas if you get the required vaccination, you’ll instead be charged for each dose with no additional consultation fee.
That said, the price will also differ depending on the vaccine and the number of doses you need. For example, let’s take the rabies vaccination. At a Superdrug Health Clinic, each dose is £62 and you need three doses. Therefore you’ll pay a total of £186 for the course. Another clinic may, of course, charge different prices.
So, it’s a good idea to check with your GP first and see what they offer, and then look around for the best prices to help you budget your pre-travel expenses.
Sources: The British Medical Association (BMA), NHS Travel vaccinations
In the US, most health insurance plans cover routine vaccines on the national immunisation schedule (hepatitis A, hepatitis B, herpes zoster, HPV, flu, MMR, meningococcal, pneumococcal, tetanus, diphtheria, pertussis and varicella) for free or at a low cost. You can also still get vaccinated without health insurance for little or no cost. The cost of travel vaccines, on the other hand, will depend on whether you have health insurance or not and where you get them done.
Most private health insurance plans don’t charge you for routine vaccines. Military insurance plans cover all recommended vaccines for those serving and their family members. Medicare covers several vaccines for free or at a low cost. And Medicaid covers all recommended vaccines for children, and some for adults as well.
However, whilst the cost of the vaccine is generally covered, you may sometimes be charged for getting vaccinated (as someone has to administer the shot) or for an office visit. This’ll vary from one state and one doctor to another.
With regards to travel vaccines, some private health insurance policies cover them, whilst others don’t. So, you should check your policy and talk to your doctor to see what travel vaccines they administer.
If your doctor’s office doesn’t administer the travel vaccines you need, you should then check with your local public health department. Sometimes they administer travel vaccines at a reduced rate. And, if all else fails, go to a travel clinic.
Similar to the UK, different clinics offer different prices. Sometimes you’re charged for the initial consultation, subsequent visits, the administration of the shot and required certificates, all on top of the vaccine cost. Therefore, make sure you look around different clinics near you to find the best prices.
The Vaccines for Children Program (VFC) offers all routine vaccines free of charge for children under the age of 19 who are Medicaid-eligible, that is to say, those who’re uninsured, underinsured or American Indian or Alaskan native.
Some federally funded local health centres also provide routine vaccinations based on your salary. And your state health department can direct you towards free and low cost vaccines, depending on your department’s vaccine resources.
None of these services or programs will offer travel vaccines for free. So, you should follow the advice from above and look around different travel clinics to find the best price.
Some travel vaccines are expensive. We’ve compared the vaccine prices from several travel vaccination clinics both in the UK and the US. All prices stated in the table are per dose, unless specified otherwise. The prices really fluctuate.
| Vaccines | No. of doses | Name of vaccine | Price per dose (UK) | Price per dose (US) | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Boots | MASTA | Superdrug | CityDoc | The New York Center for Travel and Tropical Medicine | Public Health Institute at Denver Health | The Washington Travel Clinic | Western Upper Peninsula Health Department | |||
| Cholera (oral) | 2 | Dukoral |
£58 |
£58 |
£28 | £37.50 | n/a | $255 | n/a | n/a |
| Combined diphtheria, tetanus and polio |
1 |
Rexavis | £35 | £35 | £32 | £39 | n/a |
$55 |
n/a |
$65 |
| Combined diphtheria, tetanus, polio and pertussis | 1 | Boostrix | n/a | £90 | n/a | n/a |
$90 |
$75 |
$70 |
$50 |
| Hepatitis A |
1 |
Avaxim / Havrix Monodose / VAQTA | £59 | £59 | £55 | £80 | $110 | $105 | $100 | $70 |
| Hepatitis A (child) |
1 |
Harvix Junior Monodose / VAQTA Paediatric | n/a | n/a | £50 | £80 | n/a | n/a | n/a | $45 |
| Hepatitis B | 3 | Energix B | £50 | £50 | £45 | £55 | $95 | $95 | $80 | $80 |
| Hepatitis B (child) | 3 | Energix B | £27 | £31 | £27 | £30 | n/a | n/a | n/a | $35 |
| Combined hepatitis A and B |
3 or 4 |
Twinrix Adult | £80 | £80 | £77 | £88 | $115 | $145 | n/a | |
| Combined hepatitis A and B (child) |
2 or 3 |
Twinrix Paediatric | £47 | £60 | £47 | £52 | n/a | n/a | n/a | n/a |
| Combined hepatitis A and typhoid |
1 |
ViATIM | £89 | £91 | £85 | £98 | n/a | n/a | n/a | n/a |
| Japanese encephalitis | 2 | Ixiaro | £98 | £89 | £89 | £108 | $325 | $255 | $345 | (call for quote) |
| MenACWY | 1 | Menveo / Nimenrix | £50 | £50 | £50 | £55 | $165 | $155 | $160 | $150 |
| MMR | 2 | MMRVaxPRO / Priorix | £45 | n/a | £45 | £50 | $125 | $115 | $120 | $80 |
| Polio | 1 | IPV | $90 | $70 | $60 | $40 | ||||
| Rabies | 3 | Rabipur | £62 | £60 | £58 | £69 | $425 | $385 | $415 | (call for quote) |
| Tick-borne encephalitis |
2 or 3 |
TicoVac | £65 | £65 | £65 | £72 | $345 | n/a | $375 | n/a |
| Tick-borne encephalitis (child) |
2 or 3 |
TicoVac junior | £65 | £65 | £65 | n/a | n/a | n/a | n/a | n/a |
| Typhoid (injection) | 1 | TyphimVi | £35 | £35 | £32 | £39 | $115 | $110 | $125 | $115 |
| Typhoid (oral) | 3 | Ty21 |
£35 |
£35 |
n/a | £39 | n/a | $110 | $150 | n/a |
| Yellow fever | 1 | Stamaril | £65 | £62 | £60 |
£72 |
$195 | $210 | $260 | $185 |
| Consultation | – | – | Free |
Free £20 if no vaccines or tablets are purchased |
Free £20 if no vaccines or tablets are purchased |
£15 booking fee + £10 if no vaccines or tablets are purchased |
Pre-travel consultation charge: $85 ($195 via telephone) + fee to confirm appointment: $25 |
Not mentinonned on website |
$45 (one vaccine, no consultation or prescriptions requested), $80 (regular fee, full consultation and covers prescriptions), $130 (family rate), $0 (follow-up visit for additional vaccines / to complete vaccine series), $20 (follow-up visit for prescriptions) |
$25 – $45 |
*Prices 2022
Several non-vaccine-preventable diseases pose a risk to travellers’ health.
Firstly, there’s malaria, dengue and chikungunya which are spread by mosquitoes, as well as zika, which can also spread during unprotected sex with a person infected by the virus. Mosquitoes carrying these diseases are present in most tropical and equatorial areas that are humid.
In risk areas, preventing mosquito bites is the best way to protect yourself. You must make sure you avoid mosquito bites.
On this website, we’ve published an entire article dedicated to the subject of malaria. There, you’ll find detailed information on the symptoms, types of malaria, risk areas, those most at-risk, preventative treatments, protection against mosquitoes, post-exposure treatment and much more.
All around the world, you also need to protect yourself from sexually transmitted diseases, such as AIDS, by using condoms.
There are more types of diseases that can be passed on to humans, but the risk of “catching them” is pretty low for travellers.
COVID-19 has lurked for a little too long in our lives now. What’s worse, the rules and recommendations surrounding vaccination against COVID-19 are constantly changing, particularly when it comes to travelling abroad.
However, at the time of writing this article, many countries have either fully or partially got rid of the restrictions linked to COVID-19. Brits and Americans can now enter most countries around the world without proof of vaccination against COVID-19.
Sometimes you may still need to do a test before arrival to prove that you’re negative. Or, some countries may require you to be vaccinated and have a negative test. But, in most European countries, there are no more restrictions, neither on arrival nor within the countries themselves.
Nonetheless, we know too well that this could change at any moment! So, in this section, we’ll outline the COVID-19 vaccination, testing and quarantine rules and requirements for UK and US citizens travelling abroad.
The NHS currently recommends two doses of a WHO-approved COVID-19 vaccine 8 weeks apart, followed by a booster dose at least 3 months later. However, most countries allow you to enter if you’ve had the primary course (i.e. first two jabs).
You should make sure you get your first two jabs far enough in advance. Most countries only consider you “fully vaccinated” if you had your second dose at least 14 days before travel. So, like everything else, don’t leave your vaccinations until the last minute.
The NHS COVID Pass is a handy tool that allows you to prove your COVID status when travelling abroad. You can either get a digital pass via the NHS App or online from NHS.UK, or a paper pass in the form of a letter.
To find out more about the NHS Pass and how to use it, go to the GOV.UK page or the NHS COVID Pass page.
Both passes show your vaccination records, including booster vaccinations, and / or proof of recovery from prior COVID-19 infection. To prove prior COVID-19 infection, you need to have tested positive on an NHS PCR test in the last 180 days.
If you’re a vaccinated UK citizen and are travelling abroad, you should check the GOV.UK Foreign travel advice for all the countries you intend on visiting, or even just travelling through. When you click on a country, you’ll be able to find out whether you need to show proof of your vaccination status and / or proof of recovery from COVID-19, and sometimes a negative COVID-19 test as well.
Again, the first thing you should do is check the GOV.UK Foreign travel advice for all the countries you intend on visiting or travelling through, and see their requirements for not fully vaccinated or unvaccinated travellers.
If you haven’t had all the required COVID-19 jabs, as well as providing proof of your first dose, you may also need to provide proof of a negative COVID-19 test before you travel. Then, you may be required to do another test on arrival, and then potentially have to quarantine. But, as usual, this all depends on the country you’re travelling to, so make sure you check the foreign travel advice pages.
Generally speaking, if you’re not (fully) vaccinated, most countries require a negative COVID-19 test. However, they don’t always require the same test. For example, some will accept antigen tests (also known as lateral flow tests), whereas others will require a PCR test. Each country’s travel advice page will specify which type of test you need to do.
If you need to show proof of a negative PCR test, it usually needs to be done no more than 72 hours before travel. And if you need to show proof of a negative antigen test, it should be done no more than 48 hours before travel. But, as mentioned before, these requirements change from one country to another.
If you need to provide proof of a negative COVID-19 test, firstly beware that you can’t use NHS tests for this, nor home test kits. You have to use a private test provider, whether this be in person or at home, and have the result verified by a healthcare professional, laboratory or testing site. To find a private test provider in the UK, click here.
Secondly, depending on the postage service and company used, it could take a couple days to receive your results. So, make sure you do them in time, but not so far in advance that your test is no longer valid.
US travellers should check the CDC COVID-19 website for the latest information on travelling abroad. Firstly, the CDC advise you to be up-to-date with your COVID-19 vaccinations before international travel.
Secondly, they advise you to check the COVID-19 situation in the countries you plan on visiting. You can do this via the COVID-19 Travel Recommendations by Destination page or the Travelers’ Health Destinations pages.
Thirdly, the CDC recommend looking up the entry and exit requirements for the country you plan on visiting, or even just travelling through. All this information can be found through the Travel.State.Gov Travel Advisories, particularly the COVID-19 Country Specific Information page. When you select a country, you’ll be able to find out whether you need to show proof of your vaccination status, proof of recovery from COVID-19, or a negative COVID-19 test in order to enter that country.
The CDC currently recommends two doses of a COVID-19 vaccine 2/3 to 4 weeks apart (depending on the vaccine), followed by a booster dose at least 4/5 months later (depending on your age). Or, if you have the Johnson and Johnson’s Janssen vaccine, then just one dose, followed by a booster 2/4 months later.
You’re considered fully vaccinated two weeks after vaccination. So, most countries allow you to enter if you’ve had the primary course (i.e. first two jabs and no booster) at least two weeks before travel. Therefore, make sure you get your first two jabs (or single-dose) far enough in advance.
In the US, there’s currently no standard digital health pass. However, you can use your paper CDC Vaccination Card, given to you when you get your COVID-19 vaccine, as proof of your vaccination status.
If you’ve lost your Vaccination Card or don’t have a copy, you should contact your vaccination provider to request one.
Again, the first thing you should do is check the CDC COVID-19 website for the latest information on travelling abroad. You should also check the Travel.State.Gov Travel Advisories, particularly the COVID-19 Country Specific Information page, for the entry and exit requirements for the country you plan on travelling to.
If you haven’t had all the required COVID-19 jabs, as well as providing proof of your first dose, you may also need to provide proof of a negative COVID-19 test before you travel. Then, you may be required to do another test on arrival, and then potentially have to quarantine. But, as usual, this all depends on the country you’re travelling to, so make sure you check the foreign travel advisory pages.
Generally speaking, if you’re not (fully) vaccinated, most countries require a negative COVID-19 test. However, they don’t always require the same test. For example, some will accept antigen tests, whereas others will require a PCR test. Each country’s travel advisory page will specify which type of test you need to do.
If you need to show proof of a negative PCR test, it usually needs to be done no more than 72 hours before travel. And if you need to show proof of a negative antigen test, it should be done no more than 24 to 48 hours before travel. But, as mentioned before, these requirements change from one country to another.
If you need a test to prove your negative COVID-19 status, go to the US Department of Health and Human Services (HHS) to find a COVID-19 testing site near you. Tests are available from pharmacies and health centres.

